 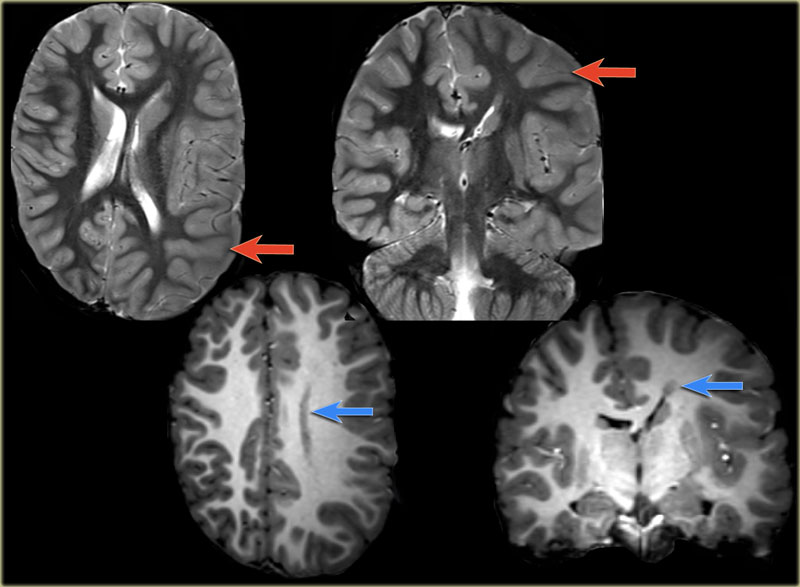
These arousals were preceded by periodic epileptiform activity that evolved to a generalized rhythmic delta activity frequently associated with persistent occipital periodic activity, a pattern that may suggest seizures, although it does not fulfill all neurophysiologic criteria. The patient had frequent arousals with evident subtle and varied, motor manifestations (brief myoclonus, discrete movements of arms and legs, swallowing movements), and occasional somniloquy with no understandable content and even shouting ( Video 1). On v-PSG, bursts of frequent brief periodic bilateral independent (right predominance) occipital epileptiform activity was detected, both in REM and NREM sleep (Figure 1). Given the previous history of meningiomas a video PSG with full 10-20 EEG montage was performed, in order to rule out epilepsy. He stopped rotigotine and piribedil, and melperone was changed to quetiapine 200 mg/d, with resolution of hallucinations and delusions, but the abnormal sleep behaviors persisted. At this time, he was on LDOPA/carbidopa/entacapone (300 mg levodopa)/day, rotigotine (4 mg/d), piribedil (100 mg/d), melperone (25 mg/d), and cyproterone acetate (100 mg/d). These features had started one year before, associated with excessive daytime sleepiness and snoring. He never reported other daytime epileptic seizures. These hallucinations were complex, not clearly stereotypical in content and they lasted long periods of time, unlike typical epileptic seizures. He also presented nightmares, daytime and nighttime visual and auditory hallucinations (description of people, associated with intense fear sensation), and occasional periods of persecutory delusions. Sometimes he had vivid dreams with associated dream enactment. The patient did not recall his movements. Straightforward stereotypy, dystonic posturing or automatisms were not reported by caregivers. These happened almost all nights, more than once per night, and were described as arm or leg movements, which sometimes were brisk like punching and kicking, and other times were like brief and low amplitude arm movements, with no apparent purpose. Įighty-year-old man, with a PD for 8 years, PD-associated dementia for the last 3 years (Mini Mental State examination of 14, due to orientation, memory and attention errors), right frontal and left parietal meningiomas, treated testis neoplasm (2008), and nephrolithiasis, was observed due to abnormal sleep behaviors. 
Some studies indicate that epilepsy and RBD may coexist, but this information is very scarce. Motor and verbal automatisms associated with temporal lobe seizures may mimic the gesturing and somniloquy observed in RBD. The hyperkinetic motor manifestations reported in frontal epileptic seizures can be reminiscent of the brisk and violent arm and leg movements seen in RBD. These clinical similarities between RBD and nocturnal epileptic seizures may result in misdiagnosis. It can mimic focal epileptic seizures, mainly frontal and temporal lobe seizures. RBD is a parasomnia with a motor and behavioral pattern frequently associated with synucleinopathies. RBD: REM Sleep Behavior Disorder PD: Parkinson's Disease v-PSG: Video-Polysomnography REM: Rapid Eye Movement NREM: Non- Rapid Eye Movement REM sleep behavior disorder, Parkinson disease, Seizures This case raises awareness for a possible role of epileptiform activity in patients with a REM sleep behavior disorder-like symptomatology. He was started on antiepileptic drugs, with improvement of the abnormal sleep behaviors. 
During REM sleep no loss of atonia nor abnormal behaviors were detected. Video-polysomnographic showed periodic bilateral occipital epileptiform activity that occurred near arousals, where subtle movements were detected. We report a case of a man with Parkinson Disease diagnosis and parietal and frontal meningiomas who started to have abnormal sleep behaviors, suggestive of REM sleep behavior disorder. REM sleep behavior disorder shares some clinical similarities with nocturnal epileptic seizures, which can result in misdiagnosis. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
